By Dr. Oren Gersten

It’s important not to understate the seriousness of the health crisis we are currently experiencing. Life has been turned up-side-down for families around the world. In our own neighborhoods people are experiencing food insecurity, loss of income, and fear of becoming gravely ill.
In the age of the internet and mass media, information is readily accessible. Infectious disease and public health experts are disseminating important information alongside bloggers, commentators, and speculators. Primary care doctors have a unique view into this situation. We are experienced in treating various diseases but also taking a holistic view on human health.
There will be no statistics or new COVID data shared in this article. This is simply a local doctor’s perspective on where we are and how we can understand our collective situation.
Health Care
COVID has taken over our health consciousness. The majority of our resources are dedicated to halting the spread of disease. Most primary care clinics have scaled back and turned to tele-health. Elective procedures have been cancelled. The irony is that all of the health problems that were present before the pandemic are still there. Some are event amplified.
We are being forced to re-assess what is truly necessary. This is not all bad. If telemedicine is a good idea in the time of COVID, health systems may adopt it after the pandemic is over to ease communications with patients and relieve the burden of frequent office visits.
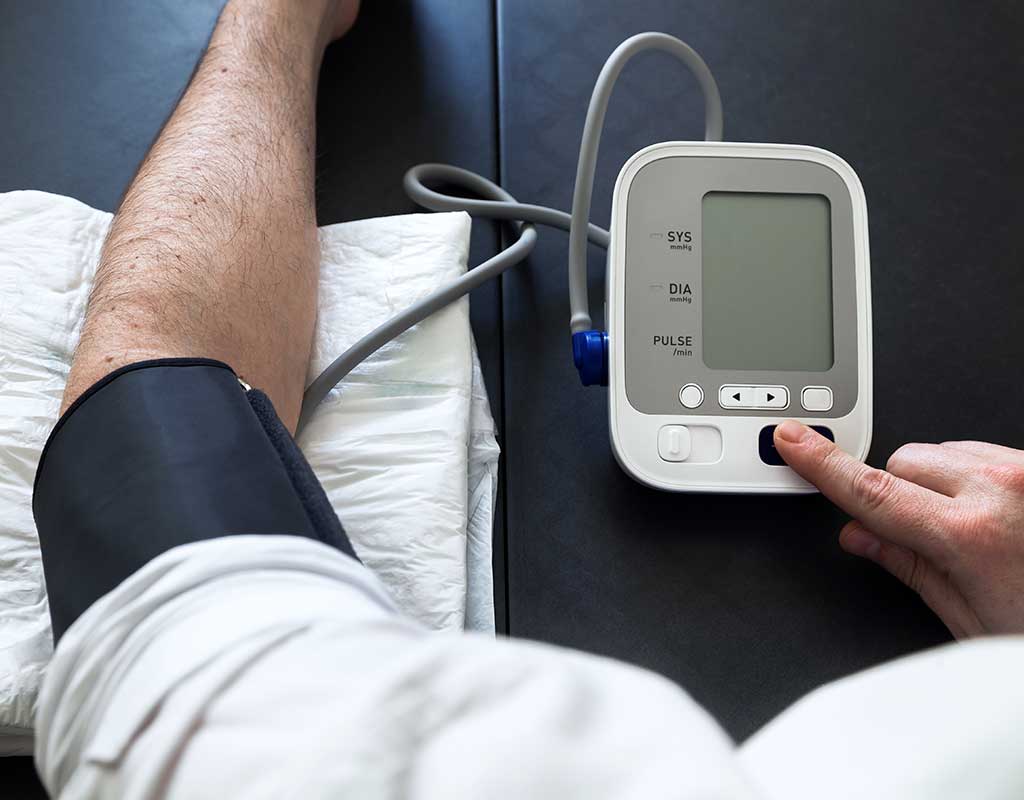
We are also realizing that patients are able to care for and monitor their health conditions with guidance rather than in-person directives from doctors. For example, accurate and easy to use home blood pressure cuffs are being used by patients with hypertension to manage this condition remotely.

I also worry about what effect isolation will have on people’s food choices. We already know that unhealthy diets are a major driver of the many modern ills, such as high cholesterol, high blood pressure, diabetes, stroke, and heart disease. Shortages in both money and fresh foods may further exacerbate these issues.
Community Support
Even before social distancing became the norm many of our friends and neighbors were already feeling isolated. Especially in elderly populations loneliness had been shown to have major detrimental health effects.
Community funds are being set up to help support families who have lost income. In medicine we call income Socioeconomic Status. This is known to be a Social Determinant of Health. In general people with less income have worse health outcomes. We need to pay special close attention to vulnerable populations during this health crisis.
Some of the most vulnerable among us are the homeless. Often suffering from chronic disease, crowded living conditions, and lack of good nutrition homeless people can be more easily susceptible to infection. Some cities in the U.S. are paying to house homeless people in hotels during COVID.
Action Steps
In addition to CDC recommendations, consider the following steps to increase your wellness during the time of COVID:
- Limit media exposure to 1 or 2 trusted sources for less than an hour a day.
- Continue self-care activities like healthy eating, exercise, and adequate sleep.
- Consider helping a neighbor or community member however you can. Altruism can help the giver and receiver to feel better.
- Try common sense solutions for health concerns first, if you are concerned ask a professional.
- Think about what we can do individually and collectively to improve the world both during and after this crisis.






